
Endometriosis


With treatment pregnancy is possible. Women who had their endometriosis treated had a pregnancy rate of 31 percent versus only 18 percent in the untreated group.
What is endometriosis and who does it affect?
Affecting one in 10 women worldwide and more than 5 million women in the U.S., endometriosis is a disorder that occurs when cells similar to endometrial cells (uterine lining cells) exist outside of the uterus. These displaced cells act as though they are part of the uterus, by swelling and thickening, then bleeding with each menstrual cycle.
Endometrial cells can also occur in fallopian tubes or ovaries – and rarely on surrounding organs in the abdomen, such as the intestines, bladder or rectum. Endometriosis can cause pain – sometimes severe – and fertility problems also may develop. Because endometriosis runs in families, it may be genetic.
What are the symptoms?
Each month, endometriotic tissue (endometrial cells that are outside of the uterus) swells, thickens and bleeds, but has no way to exit the body. The tissue becomes trapped and affects surrounding tissue, causing irritation. It can lead to adhesions and scar tissue that can worsen over time. Symptoms may include:
- Pelvic pain
- “Killer cramps”
- Long and heavy periods
- Painful bowel movements
- Low back pain
- Pain associated with sexual activity
- Infertility
![]() Pain severity isn’t necessarily a reliable indicator of the extent of the condition. Some women with mild endometriosis have extensive pain, while others with advanced endometriosis may have little pain or no pain at all.”
Pain severity isn’t necessarily a reliable indicator of the extent of the condition. Some women with mild endometriosis have extensive pain, while others with advanced endometriosis may have little pain or no pain at all.”
If I have endometriosis, will I be able to have children?
Endometriosis affects about one-half of women with infertility, but the good news is that treating endometriosis significantly improves the ability of women with this condition to get pregnant. Treatment to improve fertility entails removing the lesions, adhesions caused by inflammation due to endometriosis, or the endometrioma – a type of cyst formed when endometrial tissue grows in the ovaries – through laparoscopic surgery. In many cases, this is followed by in vitro fertilization (IVF). Approximately 17 percent of women who have trouble getting pregnant have endometriomas.
How can endometriosis be treated?
Endometriosis is treated either medically, surgically, or a combination of both. Treatment is directed at pain control, halting the progression of disease, and infertility treatment. Since endometriosis can vary widely from patient to patient, treatment must be tailored to each individual, depending on her specific conditions and goals.
Minimally invasive surgery is the best treatment, but there is no cure for endometriosis. If implants are left behind, women can still experience pain.
When is surgery necessary to treat endometriosis?
Surgery is often performed for acute pain, when medical treatments no longer work, if there is a pelvic mass, and when women have trouble getting pregnant.
Surgery for endometriosis is divided into two categories: conservative management and definitive management.
Conservative – For women with milder symptoms or those who wish to become pregnant, conservative surgery is used to remove endometriosis tissue (endometriosis excision) and improve symptoms. This form of surgery preserves the uterus, tubes and ovaries as often as possible and is commonly followed by medical therapy to prolong the length of pain control.
However, 40 percent to 80 percent of women will experience a recurrence of pain within two years of conservative surgery.
Definitive – The definitive approach is a hysterectomy with or without removing the ovaries. This treatment course is recommended for women who don’t wish to become pregnant or have severe pain that has not been successfully treated with medication and conservative surgery. A hysterectomy that removes both ovaries produces the best long-term pain control.
What are the new surgical advances to treat endometriosis, and what benefits do they offer compared to other procedures?
DualPortGYN is a new minimally invasive GYN surgical technique developed by the specialists at The Center for Innovative GYN Care that improves the overall outcome of GYN surgery. Women with complex conditions are able to have surgery with only two tiny incisions, no bigger than a paper cut – one at the belly button and one at the bikini line. While the incisions are small, complicated conditions like large fibroids, an enlarged uterus or pelvic adhesions can all be treated with DualPortGYN.
Using two additional advanced techniques, retroperitoneal dissection and uterine artery ligation, surgeons can map the entire pelvic cavity and control blood loss. Most surgeries are performed in under an hour, in an outpatient setting.
How long is recovery?
Recovery times vary from one week to 6-8 weeks depending on the type of surgery. This chart details recovery time for a variety of GYN surgical techniques.
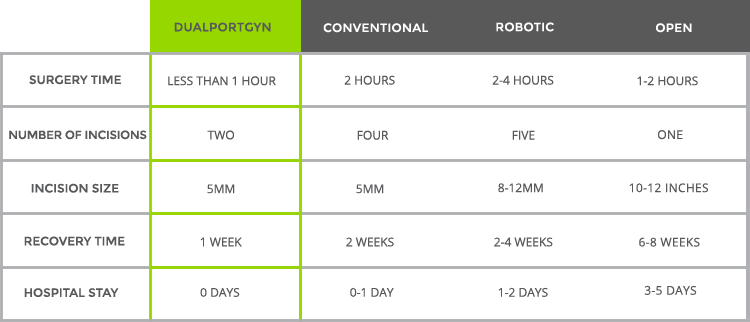
Are there alternatives to surgery?
Endometriosis symptoms may be managed medically to reduce pain symptoms (acetaminophen or ibuprofen), and some patients find relief through hormone suppression (birth control). However, medications are only used to treat the symptoms. Improving fertility and removing adhesions and endometriosis tissue requires surgical treatment. While it can be managed, there is no cure for endometriosis.
What should I ask my doctor or OB-GYN if he/she recommends surgery for endometriosis?
Before undergoing surgery, you will likely have many questions for your physician or surgeon. View our recommended questions to ask – and background information to help you weight the answers – below or download a printable version.
HOW WILL THE SURGERY BE PERFORMED?
First, if your physician recommends a hysterectomy, be sure to ask what other more conservative options are available to treat your symptoms if you would like to have children in the future. Depending on the severity of endometriosis, other surgical options exist such as minimally invasive endometriosis resection.
If a hysterectomy is the right choice for you, there are many options to consider. Sixty percent of hysterectomies in America are still performed as open abdominal surgeries. This procedure can result in severe pain, higher complication rates, and a longer recovery period than new minimally invasive procedures. Other clinics or hospitals use robotics, which require more incisions and more scarring. If your physician recommends these options, consider seeking out a second opinion before agreeing to the surgery.
HOW MANY TIMES HAVE YOU PERFORMED THIS SURGERY?
When it comes to any form of surgery, training, skill and practice matter, which is why GYN surgeons who specialize in minimally invasive surgery are the most qualified. The reality is that OB-GYNs are highly skilled obstetric practitioners, but very few perform GYN surgeries often enough to be surgical specialists. This is borne out by studies, which find that GYN surgery is commonly a secondary component of what an OB-GYN does.
WHAT HAVE OTHER PATIENTS EXPERIENCED AFTER THIS PROCEDURE?
Robotic, open and conventional laparoscopic GYN surgeries can lead to longer recovery times, increased blood loss and larger scars than newer procedures. Make sure your surgeon is trained in the latest minimally invasive techniques, such as The Center for Innovative GYN Care’s DualPortGYN, that prevent injury to the pelvic structures and minimize blood loss – resulting in reduced complication rates and improved recovery times.
HAVE YOU RECEIVED FELLOWSHIP TRAINING IN MINIMALLY INVASIVE GYN SURGERY?
While most OB-GYNs are highly trusted generalists, they spend most of their time focusing on obstetrics and basic GYN care and therefore, perform specialized GYN surgeries rarely. Be sure to choose a surgeon who has received comprehensive training and performs many endometriosis resections or minimally invasive hysterectomies to treat endometriosis each year.
WILL POWER MORCELLATION BE USED TO REMOVE TISSUE DURING THE SURGERY?
This is an important question when considering gynecological surgery. The reason is because hidden uterine cancer called sarcoma can be spread through the abdomen and pelvis during surgery when the small motorized blades in these devices spin at high speed to cut the tissue into small strips for removal. The Food and Drug Administration (FDA) now requires all surgeons to tell women in advance if the surgery involves a power morcellator and to get written consent before the surgery takes place.
WILL ROBOTICS BE USED TO ASSIST WITH THE SURGERY?
Although the American Medical Association and other leading medical societies have issued statements discouraging robotic techniques due to much higher costs to patients without any medical advantages, robotics continue to be used in GYN surgeries. This is because robotic procedures “enable” an OB-GYN not well trained in laparoscopic GYN surgical techniques to complete a procedure through a “minimally invasive” approach. This is why women need to ask if robotics will be used during a GYN surgery and to seek a specially trained surgeon able to perform the latest minimally invasive surgical techniques for endometriosis, such as DualPortGYN and retroperitoneal dissection, that do not use robotics.
WHAT IS MY ANTICIPATED RECOVERY TIME?
New minimally invasive GYN surgical techniques require, on average, only a week to recover. Other procedures such as open abdominal surgery can take up to 8 weeks.
WHAT ARE MY OTHER SURGICAL OPTIONS?
Ask your physician if he or she is aware of new, minimally invasive procedures.
Women need to be their own best advocate, which is why getting a second opinion is always good practice. Since there are different surgical options for treating endometriosis, getting a second opinion is a way you can ask questions about how the surgery will be performed, the recovery time, and possible complications.


